Your Ultimate Guide to Selecting a Healthcare Revenue Cycle Management (RCM) Vendor
Looking to outsource your hospital's revenue cycle management? Explore the criteria to look for in a comprehensive RCM.
Revenue cycle management (RCM) is a complex process that can significantly impact the financial health and reputation of a healthcare provider.
Denials are common. The rise in out-of-pocket medical bills results in lower collection rates and higher bad debt. Adding to this challenging environment, errors in the revenue cycle often delay reimbursement from insurers and patients.
What if there was a way to help increase provider revenue and improve patient experience? An
RCM vendor partner can help to create a more positive outlook for the future. But not all RCM
vendors are created equal. Here are some key considerations to make before selecting an RCM
vendor partner.
Identify Your RCM Needs
Before you start evaluating potential vendors, it’s important to identify your specific needs and priorities. Consider your organization’s current pain points and the features and capabilities you need in a new system.
 |
 |
 |
| Are you looking to streamline your billing processes? |
Improve your financial reporting? |
Or enhance patient engagement? |
Having a clear idea of your requirements will help you select a vendor provider that's the proper fit for your organization. After you understand your needs better, the next step is to ask specific questions to assess potential RCM vendors.
1. What are the RCM vedor’s specialties and expertise?
You’ll want to look for a vendor partner with a strong track record of success and a clear understanding of the complexities and nuances of healthcare billing.
When vetting potential vendors, inquire about their experience in areas such as claims management, denials management, collections, and payer contract negotiation. Also, check their understanding of the regulatory environment, as this can affect how effectively they can support your organization. A vendor with the right expertise and experience will be a valuable partner in helping you navigate the revenue cycle and achieve your financial goals.
2.What is their experience with healthcare systems like yours?
You’ll want to find a partner with experience working with healthcare providers similar to yours in size, specialty, and complexity. This will ensure that they understand your unique needs and can tailor their services to meet your requirements.
3.How does the provider plan to work with your existing systems and processes?
In addition to comparing how different RCM vendors integrate with your existing systems, you should also ask about their onboarding and implementation process. How long will it take to get up and running with your organization? What kind of training and support will they provide for your team? How will they help you through the transition, and what kind of ongoing support can you expect?
4.How does the vendor ensure compliance with changing medical billing regulations?
Everyone who works in healthcare administration knows that change is a constant when it comes to regulations. The RCM vendor should have a comprehensive understanding of HIPAA, CMS, and other relevant regulations and be able to clearly explain how they ensure compliance. Ask about their training and education programs, compliance audits, and how they handle any potential violations.
5.What is their pricing structure, and how does it align with your budget?
You’ll want to understand the provider’s pricing structure and ensure it aligns with your budget and financial goals. Make sure to dig deeper into the fine print to uncover any additional fees or hidden costs. While cost is an important factor, prioritize value and the potential for revenue optimization over the lowest price. The right vendor will be an investment that provides an appropriate ROI.
6.What is their implementation process and timeline?
It’s important to inquire and compare RCM vendors’ typical implementation timeline. Pay close attention to how they handle the data migration process, and what support they offer during and after this phase. It’s also a good idea to ask about their change management process and how they plan to help your staff get up to speed on the new system. With a clear understanding of the implementation process, you can plan accordingly and avoid any surprises.

Industry Certifications and Relationships Matter
An experienced RCM vendor partner should bring more than just industry knowledge and know-how to the table. They also bring valuable connections and relationships with key players in the industry, such as insurance companies and third-party payers. With these resources, they can then help you to stay compliant with the latest regulations and policies.
Check for industry certifications, which provide assurance that your provider is committed to upholding the highest standards of quality and ethics. This checklist of certifications will help you during the vetting process to properly filter through potential vendors:
RCM Vendor Certifications

AHIMA(American Health Information Management Association) certification ensures that providers have the skills and knowledge necessary to manage healthcare information. |

AAPC(American Academy of Professional Coders) certification validates providers’ expertise in medical coding. |

HFMA(Healthcare Financial Management Association) certification demonstrates providers’ understanding of healthcare financial management. |
 HFMA CRCR(Certified Revenue Cycle Representative) certification improves providers’ knowledge, competencies, and productivity in RCM, allowing them to provide best-practice recommendations for healthcare organizations. |

HITRUST CSF(Common Security Framework) certification verifies that RCM vendors have the knowledge and skills to protect information and manage risk, ensuring compliance with key regulations. The certification validates a provider’s commitment to compliance and security. |

AAHAM CRCE(American Association of Healthcare Administrative ManagementCertified Revenue Cycle Executive) certification demonstrates that providers have a deep understanding of revenue cycle management in institutional settings and the ability to optimize revenue streams for healthcare organizations. |
The Role of Technology and Infrastructure in RCM
Technologies like automation and AI are revolutionizing the healthcare revenue cycle by streamlining processes and increasing efficiency, all of which helps healthcare organizations optimize their revenue.
Robotic process automation (RPA) and cognitive automation are two key technologies that are transforming the way healthcare organizations manage revenue. RPA automates repetitive tasks, including patient scheduling, check-in, and bill pay, while cognitive automation uses machine learning (ML) and natural language processing to understand and respond to data inputs.
ML algorithms can take data analysis to the next level, detecting patterns in billing and coding data that humans might miss or not have the bandwidth to analyze. This can help to identify billing errors and optimize net revenue. In addition, by automating tedious tasks like verifying patient data or coding claims, AI and ML can free up healthcare professionals to focus on the human element of healthcare delivery, providing a better experience for patients and staff alike.
While automation is a key component of efficient revenue cycle management, it’s not the only technological factor to consider. Here are some additional considerations to check into when looking at capabilities and infrastructure:
 |
 |
|
Comparison of Contracted Rates: Do stakeholders have the ability to see how contracted rates compare across different payers? This capability will allow them to set benchmarks, forecast performance and monitor year-over-year trends. |
Valuable Insights: A good revenue cycle management program provides valuable insights into healthcare providers' revenue performance and communicates effectively with patient management systems, government programs like Medicare and Medicaid,and commercial payers. |
 |
 |
|
Proactive Identification of Issues: The best systems proactively identify and address issues that could negatively impact reimbursement, thus minimizing potential losses. |
Robust Infrastructure: A robust infrastructure ensures that the system can handle large volumes of data and transactions with 24/7 availability. |
All of these factors can have a direct impact on your organization’s bottom line as well as patient satisfaction, which makes technological functions and features an important area worth deeply exploring.

Compliance and Security
Given the sensitive nature of patient information and the complex regulatory environment, RCM companies must maintain the highest data privacy, security, and compliance standards. Because the stakes are so high for health systems when it comes to patient data and privacy, it’s crucial to make sure your RCM vendor covers all of the bases in terms of compliance and security. Each of the following safeguards and requirements should be met by your chosen vendor:
HIPAA
The Health Insurance Portability and Accountability Act (HIPAA) establishes national standards for the privacy and security of health information, including electronic protected health information (ePHI). HIPAA mandates that healthcare providers and their business associates take appropriate measures to safeguard the confidentiality of ePHI.
HITECH Act
The Health Information Technology for Economic and Clinical Health (HITECH) Act strengthens privacy and security protections for electronic health information. It requires prompt notification of any breach of unsecured PHI, and provides financial incentives for healthcare providers who adopt electronic health records and meet meaningful use requirements.
Affordable Care Act
The Affordable Care Act (ACA) includes provisions related to improving the quality of healthcare, reducing healthcare costs, and detecting and preventing healthcare fraud and abuse.
State-Specific Regulations
RCM vendors may be subject to state-specific regulations like the California Consumer Privacy Act (CCPA), so it’s best to determine which criteria need to be met within your state(s) and ensure the vendor you select can meet these guidelines.
PCI Compliance
PCI compliance ensures that any time a healthcare provider processes, stores, or transmits credit card information, it’s done so in a secure environment. This is crucial to protect patients from potential data breaches and unauthorized transactions as well as to safeguard the reputation and financial integrity of individual healthcare organizations.
Stakeholders should also evaluate the provider’s security infrastructure, policies and practices. This may include reviewing documentation such as security risk assessments, incident response plans, disaster recovery plans and security audits.

Pricing and Contracts
Several different pricing models exist for revenue cycle management services and it’s best to
compare each to find the one that suits the size and needs of your healthcare organization.
Here is an explanation of several of the most common pricing structures.

|
Fee-for-service model A common model is the fee-for-service model. This pricing model charges a percentage of the total revenue collected by the revenue cycle management company, depending on the provider and the level of services being provided. Some important considerations when evaluating a fee-for-service model include: ● How the pricing percentage is calculated. Is it based on gross or net revenue? |
|
Flat-fee model Under this pricing model, the provider charges a fixed rate for their services, regardless of the required volume or complexity of the tasks. Look for the following when evaluating a flat-fee ● What services are included in the flat fee? |
Bundled pricing
A bundled pricing model packages several services together for a single price. In addition to the
considerations noted above for fee-for-service and flat-fee pricing, here's what to look for when
evaluating a bundled pricing contract:
● What services are included and excluded in the bundle?
● Does the service-level agreement outline how the provider will ensure accurate and
timely claim submissions, follow-up, and appeals?
● Are there customized reporting or data analytics provisions in place to improve
performance and profitability?
When evaluating any RCM pricing model or contract structure, review each component carefully
to ensure that it aligns with your organization's unique needs and provides the level of support
required for successful revenue cycle management.

Implementation and Training
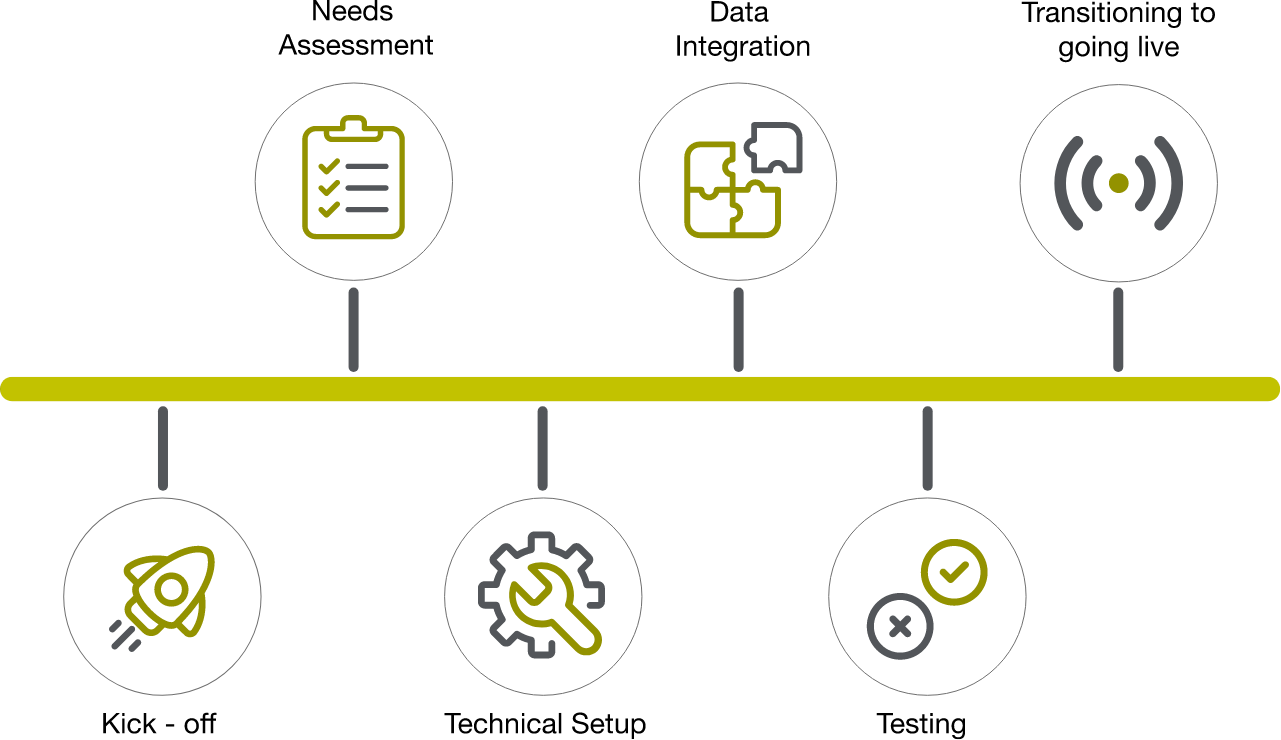
Having the right components and safeguards are only one part of the process of adopting an RCM system with a new vendor. The next stage, of implementing and training staff to efficiently utilize it, is just as important. While this journey can vary depending on your vendor partners, it universally progresses through these key six stages:
Each vendor has a different approach to this onboarding process. For instance, GetixHealth differentiates itself by delivering innovative and result-driven implementation solutions to our client partners. Our Director, Christian Wilkin, explains why this is one of our key guiding principles:


Let's unpack these steps in more detail.

|
Kick-off call: This is where the partnership journey begins. At GetixHealth, this is a strategic alignment of our top stakeholders internally and those of the client partner’s organization. At this time we set mutual expectations, timelines and the project’s scope. |

|
Needs assessment: |
|
|
Technical setup and interface integration: |

|
Data Integration: |

|
Testing and Go Live: Once set up, the system undergoes rigorous testing to ensure functional excellence and precise data processing. GetixHealth ensures that every parameter meets our stringent quality standards. It is only after this detailed process is complete, that we give the green light for the system to go live. |

|
Monitor and Evaluate: Post-implementation, the work doesn’t stop. Your vendor partner should remain committed to continually assessing the RCM’s efficacy by monitoring vital KPIs, scrutinizing data, and fine tuning strategies to elevate your revenue cycle process. For GetixHealth, we believe in a proactive approach to continuously supporting the evolution of our client partners and maintain communication to make certain their needs are being met. |

The Role of Revenue Cycle Management in Improving Patient Satisfaction
Revenue cycle management companies can ensure patient satisfaction by implementing
strategies that improve the patient experience. Here are some ways that revenue cycle management companies can achieve this:
● Help patients pay faster and in full by providing convenient payment technology and clear explanations of payment responsibilities.
● Optimize back-end claims, billing, payment, and collections processes to free up staff to provide individualized help to patients who need it.
● Improve a patient's financial experience by providing simple, accurate estimates with clear explanations prior to an appointment, along with digital self-service pay options.
● Focus on improving patient care and customer service practices, which can have a significant impact on revenue.
● Partner with third-party providers to build capabilities that improve care access and decrease out-of-pocket expenses, ultimately improving patient satisfaction rates.

Key Benefits of Outsourcing Revenue Cycle Management
Outsourcing revenue cycle management services can help healthcare organizations realize numerous benefits, both in the short and long-term.
Out of the healthcare providers that participated in the survey, a whopping 95% reported an increase in revenue, with two-thirds saying the improvement was substantial. These findings suggest that outsourcing RCM can be a real game-changer, helping to boost a provider’s bottom line and improve their financial health.
The benefits of outsourcing RCM go beyond just improving financial performance. According to the Medical Group Management Association (MGMA), facilities that outsource their RCM can also enjoy other benefits, like reduced staff turnover and improved patient satisfaction.
Outsourcing their RCM allows staff to focus on providing high-quality patient care rather than getting bogged down in administrative tasks. How could the following benefits change the landscape of your health system?

|
Improved Efficiency |

|
Enhanced Data Security |

|
Accurate Payments & Reimbursements |
A Quick Checklist For Selecting a RCM Vendor Partner
Use this list as a guide while evaluating potential RCM vendor partners and if you have any questions during your search, reach out to GetixHealth for more information. Our expert team has guided many healthcare providers through the process, so we understand the concerns and questions healthcare leaders have during the selection process.
● Do they offer automated insurance eligibility verification?
● How much experience do they have working with organizations of a similar size and
complexity?
● How satisfied are their clients?
● How do they improve Days A/R?
● What procedures do they have in place to correct billing and coding errors?
● What kind of technology do they use?
● Do they have robust data security measures and a strong privacy policy in place?
● How is their customer support team structured, and how easy is it to get help when you
need it?
● How do they stay up-to-date on industry trends, best practices, and regulations?
● What kind of training resources do they provide to ensure you get the most out of their
system?
● Do they offer any additional services, such as analytics or data-driven insights, that
could be valuable for your organization?
● What is their process for onboarding new systems and migrating data?
● What kind of reporting capabilities do they have, and how easy is it to access this
information?